New treatment offers hope for Nepal’s leprosy patients
Hospital has novel solution to heal wounds, but no cure for stigma and ostracisation
A revolutionary treatment for open wounds has dramatically reduced the healing period of leprosy patients in Nepal, saving them money and prolonged pain. The new procedure has huge implications internationally, as it reduces the medical cost for treating patients with chronic open wounds.
The technique, called Leukocyte Platelet Rich Fibrin (LPRF), was devised for dental surgery by Nelson Pinto of Chile and has proven to accelerate the healing of tissue. Now, it is also being used to treat hard-to-heal skin lesions of diabetes and leprosy patients.
“LPRF has shown miraculous results in the treatment of chronic wounds in Nepal,” says dental surgeon Sushil Koirala who is pushing the new treatment in government hospitals. “It does not need special equipment, is cheap and, so simple even paramedics and nurses can perform it.”
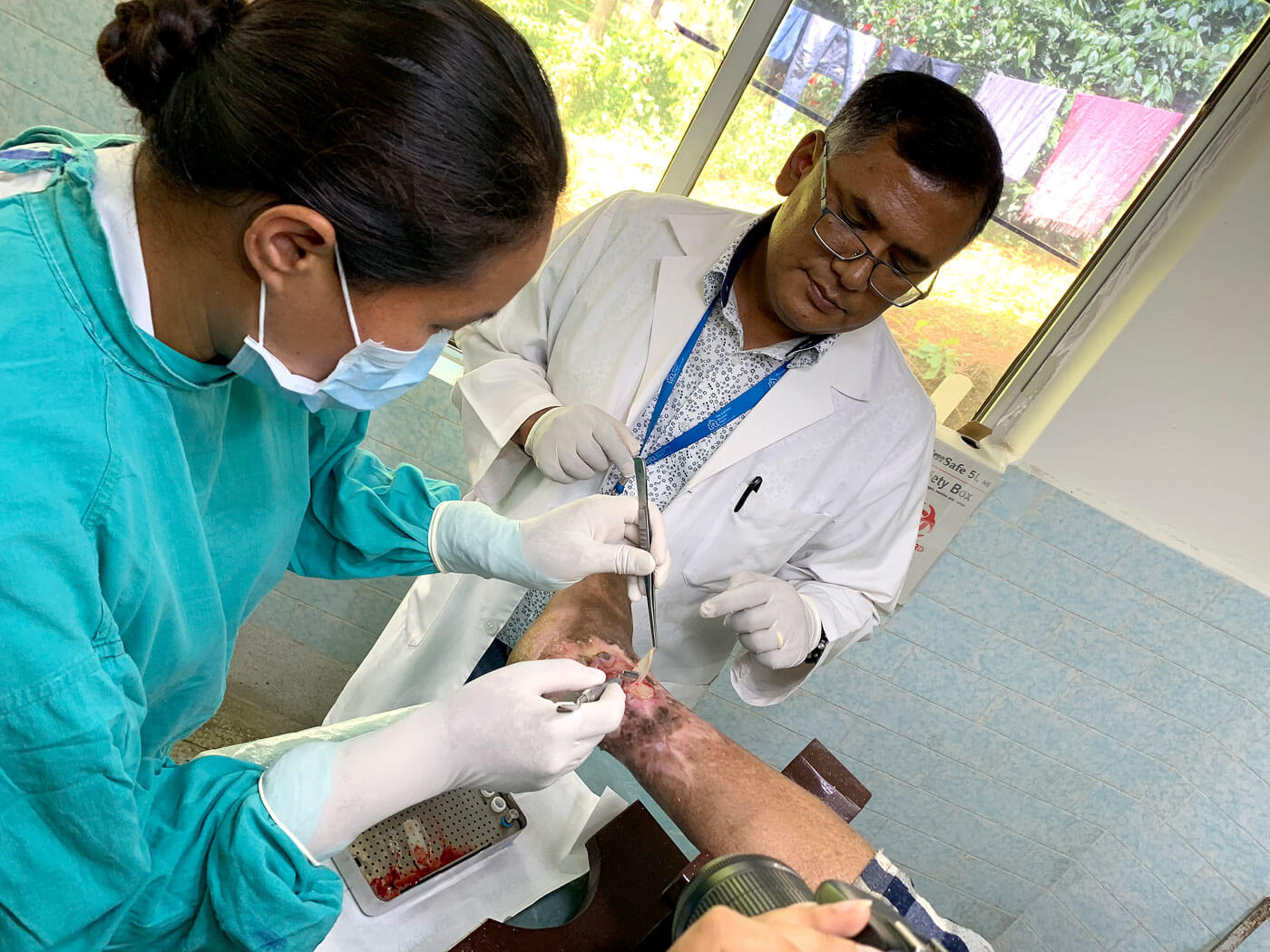
There are three specialised leprosy hospitals in Nepal: Ananadaban in Lele, Green Pastures in Pokhara, and Lalgadh in Dhanusa. Anandaban Leprosy Hospital 16 km south of Kathmandu has been trying out LPRF on patients with excellent results.
Leprosy is a biblical disease in which bacteria called Mycobacterium leprae damages the patient’s nerves and causes the fingers, toes and limbs to go numb, leading to further injuries. Leprosy is treated with antibiotics, but some patients suffer antigen reaction and need long-term rehabilitation.
One of the patients at Anandaban is Phelit Sahi, who was ostracised by her community in Jumla because she had leprosy and had been living in a cave for 25 years. Reporters who had gone to cover a local event in a helicopter found out about her, and flew her to Kathmandu for treatment.
Every week, doctors draw 80cc of blood from her and place it in a special centrifuge for 12 minutes. The clear plasma separates from the red corpuscles and is compressed to form a high-density fibrin clot which is applied to her wound.
“She is among more than 100 patients that we have treated with LPRF, and we have gained enough experience in this technique to lead the way for the world,” says surgeon Indra Bahadur Napit at Anandaban, who presented his results at WHO in Geneva.
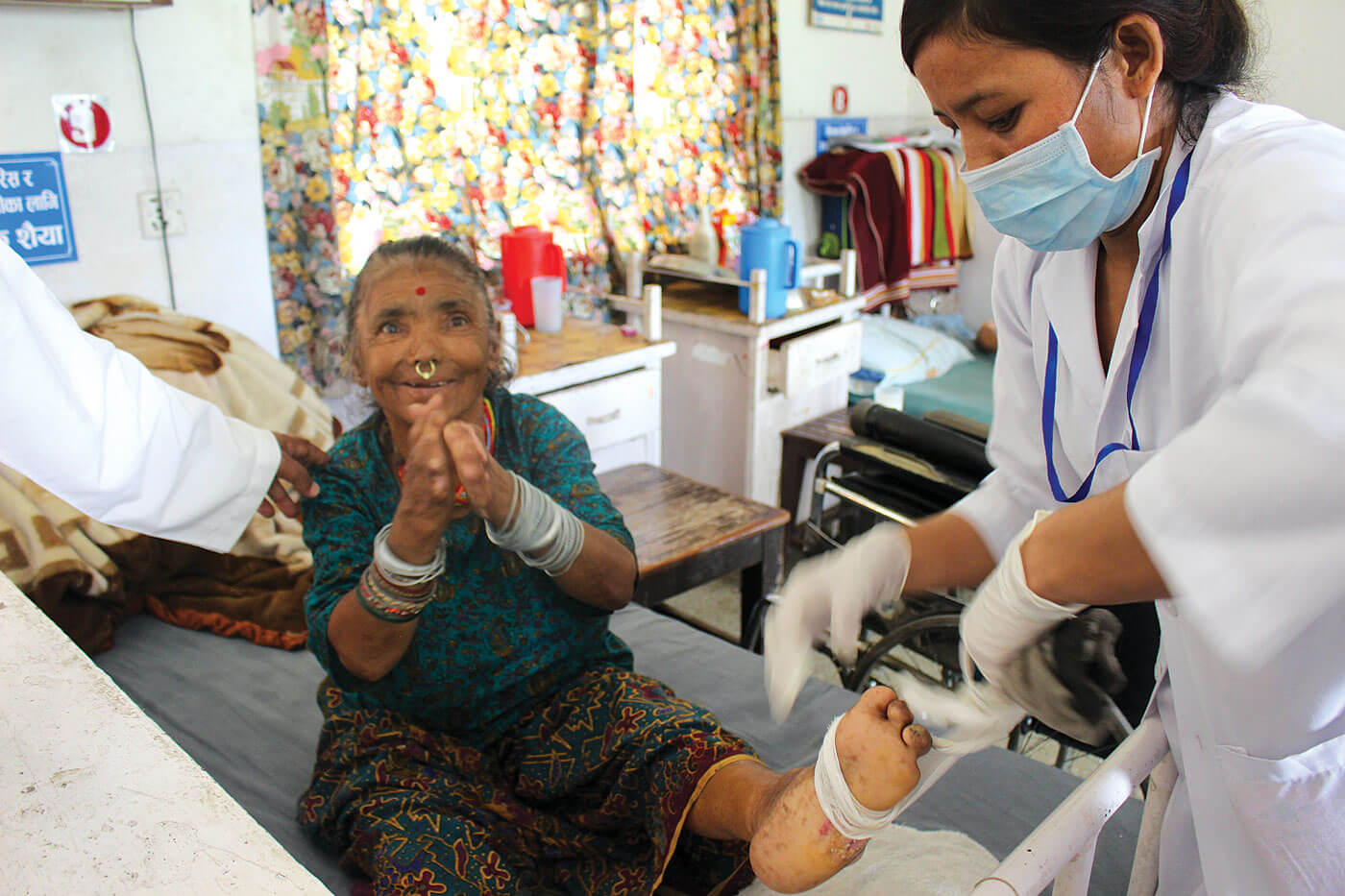
Raju Lama was 27 when he was diagnosed with leprosy, but because of late diagnosis, his fingers and toes were deformed, and he had to abandon his job. Doctors recommended amputating his right leg, but became the first patient to get LPRF treatment. He is happy with his “ragat upachar” (blood treatment) and says after several LPRF procedures his wounds are healing much faster.
Ram Kumari Sah and her husband from Janakpur have been living with leprosy for decades. She does not feel pain in her hands and legs and often hurts herself. Her lesions become infected and never healed. This week, she was waiting for her turn at the LPRF ward in Anandaban.
The hospital’s LPRF pilot study has shown that 97% of the cases healed completely within seven weeks. The results are so encouraging that news of this revolutionary treatment has spread through word of mouth. A dozen patients, currently at Anandaban were referred by hospitals in India. A team of Nepali doctors is also training doctors in Burma, Bangladesh and Nigeria.
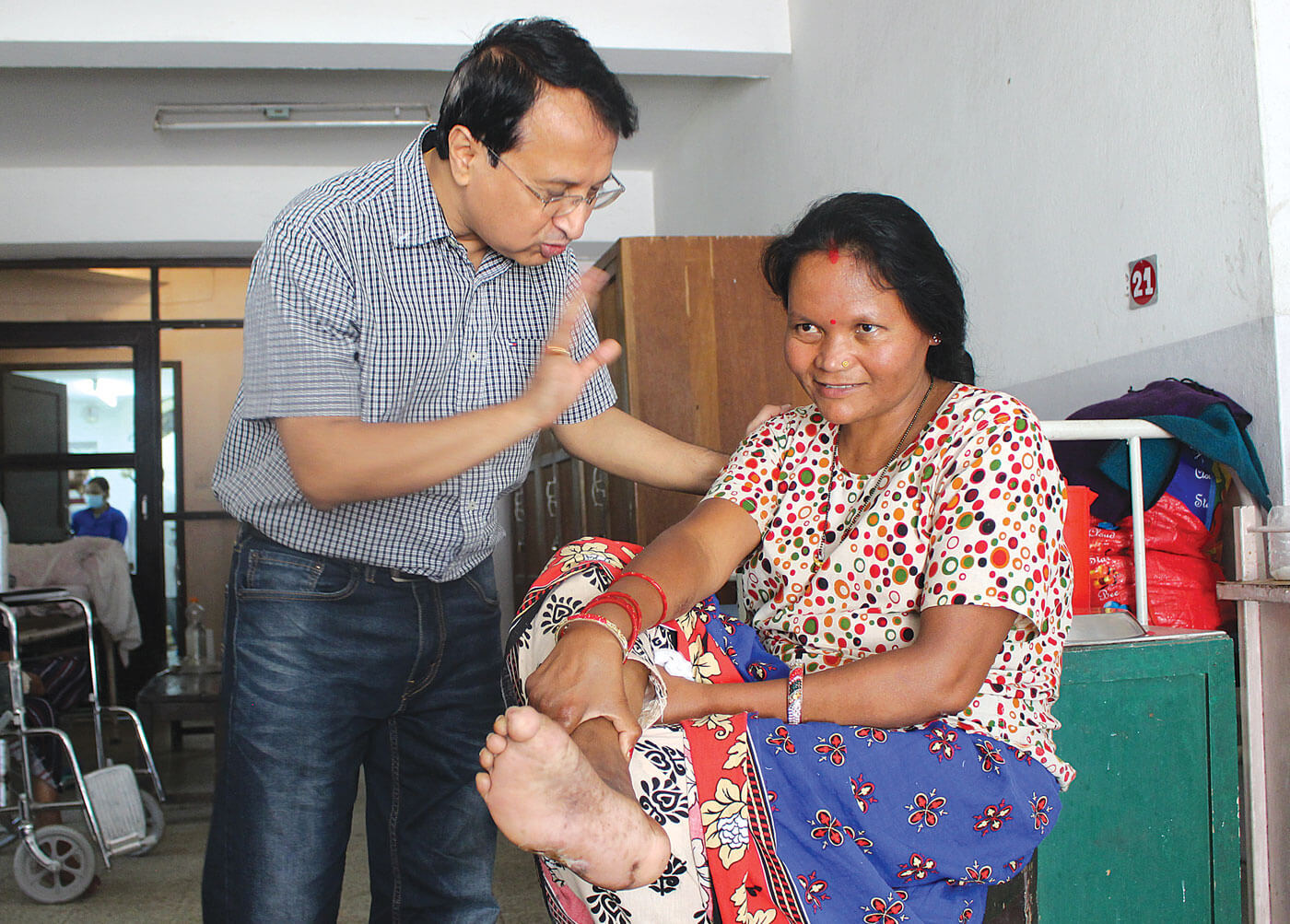
The new treatment is expected to add to Nepal’s success in reducing the prevalence of leprosy from 21 cases per 10,000 in the 1980s to less than 1 today. Nepal was officially declared leprosy-free in 2010 when the prevalence rate came down to 0.79%.
However, in recent years, the prevalence rate is creeping up again, and was 0.94% in 2018. More than 3,000 new patients are diagnosed with leprosy every year, with most of the cases found in Province 2. Experts say this could be a result of active case finding and may not mean that the prevalence is increasing.
Leprosy is curable with multidrug therapy but many do not get treatment on time. The incubation period is five years on average and symptoms may occur within a year, but can also take as long as 30 years to become visible, making the disease difficult to diagnose, and the delay leads to nerve damage and deformities. Leprosy is transmitted through the air during close and frequent contact with untreated cases.
“Leprosy can afflict anyone but there is a correlation between the disease and poverty,” explains dermatologist Mahesh Shah. “If one’s immune system is strong, the bugs do not do any damage. But poor hygiene and nutrition increases susceptibiltity. Neglected people from neglected countries suffer from leprosy the most.”

Up to 40% of patients undergoing multidrug treatment develop a reaction, and need long-term hospitalisation. Since the patients are poor, most private hospitals are not interested in treating them. At Anandaban, treatment is free as it is supported by government grants and charities.
Since 1% of cases suffer from relapse in Nepal, active door-to-door case finding is important to meet the WHO target of zero leprosy transmission by 2030.
Even more daunting is to counter societal stigma and ostracisation of leprosy patients. Family members regard the disease as punishment from the gods, and even some medical interns and nurses refuse to touch patients despite patients being on antibiotics and unable to spread the disease. Nepal’s laws still allow husbands to divorce their wives if they have leprosy.
“It is a complicated disease made even more so by stigma and ignorance,” says Napit, “but with LPRF, we now have a powerful weapon in our arsenal. A vaccine would be the final solution, but no one cares about leprosy. All the funding goes for diseases like HIV.”
Miraculous healing
When Nelson Pinto’s favourite horse broke its leg, he had two options: either put it down or amputate its leg. The Chilean dentist decided on a third option.
He drew some blood from the horse, spun it in a centrifuge to separate the autologous fibrin matrix which is rich in platelets, and applied the plasma to the horse’s wound. After a few weeks, the horse was cantering again.
Pinto knew about the technique because Leukocyte Platelet Rich Fibrin (LPRF) was developed for dental implant treatment. The surgeon was so convinced that the new process would be useful in treating chronic open wounds that he embarked on a global crusade to spread its use.
Pinto convinced fellow-dentist from Nepal, Sushil Koirala, whom he met at an international conference, to adopt the technique. Since then, Koirala has been trying to convince the government and private hospitals to adopt the procedure, but without much success. However, Anandaban Leprosy Hospital in Lalitpur has seen phenomenal improvements in the healing time of lesions among its patients. (See adjoining report above)
LPRF is now used to treat diabetic wounds, lesions caused by leprosy, localised burns and surgical wounds, and with this, healing time is often cut in half. It is also being used in cosmetic surgery to remove wrinkles and rejuvenate the skin. The reason why it is so effective, Pinto explained during a trip to Nepal last month, is because it is completely natural and autologous, which means a patient is not receiving any foreign tissues or chemicals.
And the treatment is cheap. A similar treatment used in Europe, which involves a kit manufactured by a multinational pharmaceutical company, costs $3,000 per patient. LPRF costs only $30. But it seems as though private hospitals are not interested in this treatment as patients heal so quickly. Many doctors are also not enthusiastic because LPRF can be administered by a paramedic or a nurse.
Says Sushil Koirala: “The reason they don’t like it is because there is no money in it. LPRF only uses the patient’s blood and there are no chemicals or equipment involved for multinational companies to make money out of.”
Koirala’s Punyaarjan Foundation has donated centrifuge machines to a few hospitals in Nepal including the Sushma Koirala Memorial in Sankhu, Anandaban Leprosy Hospital, Bir Hospital in Kathmandu and to three hospitals in Burma with varying degrees of acceptance.
The Bible relates how Jesus Christ miraculously and instantaneously cured ten lepers at the gates of Jerusalem. LPRF may not cure leprosy lesions as quickly, but the procedure is nearly as miraculous.
Life after leprosy

Kumar Tamang, 47, is putting the final touches on his painting of an elephant with a bejewelled crown and a howdah. He dips his paintbrush on a palate and paints the border bright red. His fingers are numb and deformed by leprosy, yet he has been painting for 25 years. His love for Mithila art is on full display on the walls, pillars and ceiling of Shanti Sewa Griha, a leprosy clinic set up by the German charity, Leprahilfe, in 1992.
Nearby, in a dark corner, is 50-year-old Nathuni Barai from Nawalparasi, who also has deformed fingers which he uses deftly to draw intricate patterns on a letter pad. Both Tamang and Barai are former patients at Shanti Sewa Griha, making a livelihood from products that Leprahilfe buys from fundraising. Their families live nearby, and their children attend a school set up by the charity.
Now, nearly three decades after the clinic was set up, Shanti Sewa Griha runs a school and orphanage in Budhanilkantha, an organic farm in Sundarijal and a rehabilitation centre near Pashupati.
As the number of patients grew, they were trained in painting, tailoring, quilt making, carpentry and jewellery making as a form of livelihood. Bags, uniforms, paintings, stationery and decorative items are sold as souvenirs to raise money for the upkeep of the shelters and to pay former patients.
“This is a form of operational therapy which tries to break the vicious circle this disease has formed,” said Marianne Grosspietsch, one of the founders of Leprahilfe. “Our goal is to create hope in Nepal.”
In 1974, Grosspietsch adopted a young boy named Puskar Limbu who had leprosy like the rest of his family. She took the boy to her home in Germany, treated his leprosy and sent him to school. Limbu went on to pursue a successful career in graphic design in Germany and is a grandfather himself today.
Children of former leprosy patients have also gone on to become nurses and doctors.
Kalpana Pariyar (pictured above) was 14 when she was diagnosed with leprosy before there was serious nerve damage to her fingers. She grew up in the shelter and married fellow-patient Krishna Majhi, whom she took care of until he died eight years ago. She now has a college going daughter and an eight-year-old son.
“I have spent my entire life here. This is my home, this is where I made my life and found peace,” says Pariyar, looking up from her sewing machine on which she was weaving dhaka fabric.
Sonia Awale
