Dengue ravaged Nepal last monsoon, with over 55,000 hospitalisations and 88 fatalities. But that is just the official count, and many who died from the mosquito borne virus that caused haemmorhagic fever were healthy adults.
Public health experts had warned last year that the virus would strike again in the 2023 rainy season because the virus hibernated with the larvae of infected mosquitos. They say the larvae are just waiting for the puddles to hatch, and with it the virus can again spread exponentially. Waiting until the monsoon to target mosquito breeding areas will be too late.
“Local government must start the search-and-destroy larvae campaign now, we cannot wait for the rains,” warns virologist Sher Bahadur Pun at Teku Hospital. “Dengue is a real public health crisis and we cannot prevent it without the government and the communities working together, individual precaution can only go so far.”
The key is to raise awareness, preferably through school children so that we can reach their families and subsequently the community at large, about the nature of aedes mosquito that carries the dengue virus and the protective measures.
Last year, almost every family in Kathmandu had multiple members suffering from dengue. Although 90% of patients were asymptomatic, they helped spread the virus.
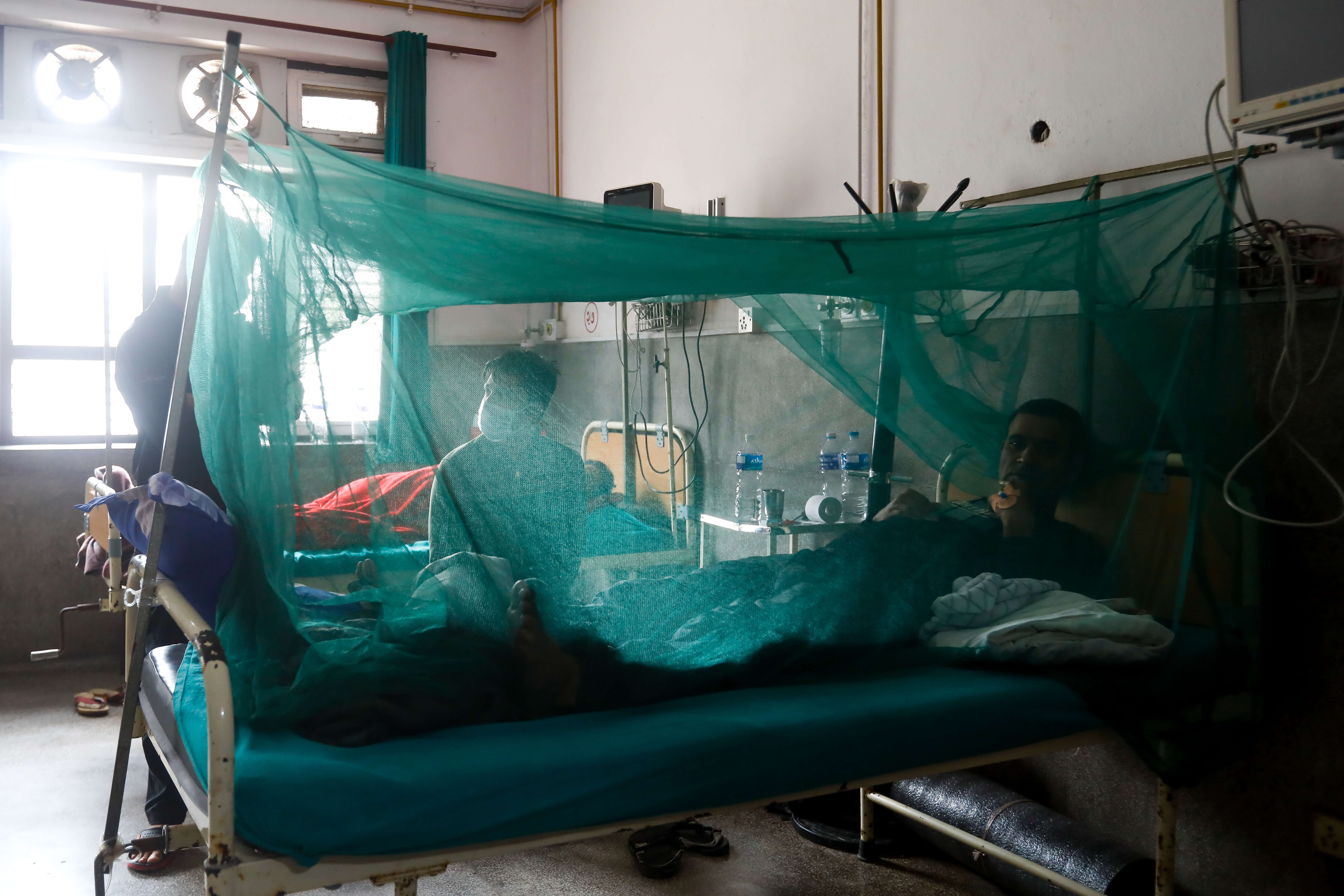
Dengue patients generally have two weeks of high-grade fever accompanied by extreme muscle and joint aches, loss of appetite, nausea, and pain in the eye sockets. Many who had both dengue and Covid said dengue was much worse.
Covid-19 is also back again, possibly with a circulation of a new variant in the region. So all three levels of government must prepare for both outbreaks simultaneously.
“Dengue is among the biggest public health challenges of the 21st century, given the disease burden and its socioeconomic impact in these parts of the world,” says Buddha Basnyat, physician at Patan Academy of Health Sciences. “And there is every potential of another outbreak given that we have not learned our lesson from previous outbreaks or taken any measures to prevent another one this year.”
Indeed, Kathmandu had a major dengue outbreak in 2019, just before Covid-19 spread out of China in December of that year. There were over 17,000 official cases that monsoon but they were largely adult patients, most of which had milder symptoms and the fatality was very low.
But last year’s outbreak was much more widespread and serious. Although debilitating, fatality from dengue is rare but there were more complications and deaths. The mosquito eradication campaign came too late, and by that point dengue was out of control.
We did not learn the lessons of 2019, and we haven’t learned the lessons of 2022.
“How not to get dengue? It is simple, do not get bitten by a mosquito,” says Pun. “But preventing a mosquito bite is anything but simple because we do not do anything until it is too late.”
Unlike the anopheles mosquito which carries the malaria parasite, aedes is active during the daytime, particularly in the early hours of the morning and evenings. This means avoiding the outdoors during these hours, if possible. So, mosquito net or coils at night do not help. Insect repellents should not be toxic, and contain the active ingredient that the aedes mosquito avoids. Full-sleeve clothes are always a better alternative.
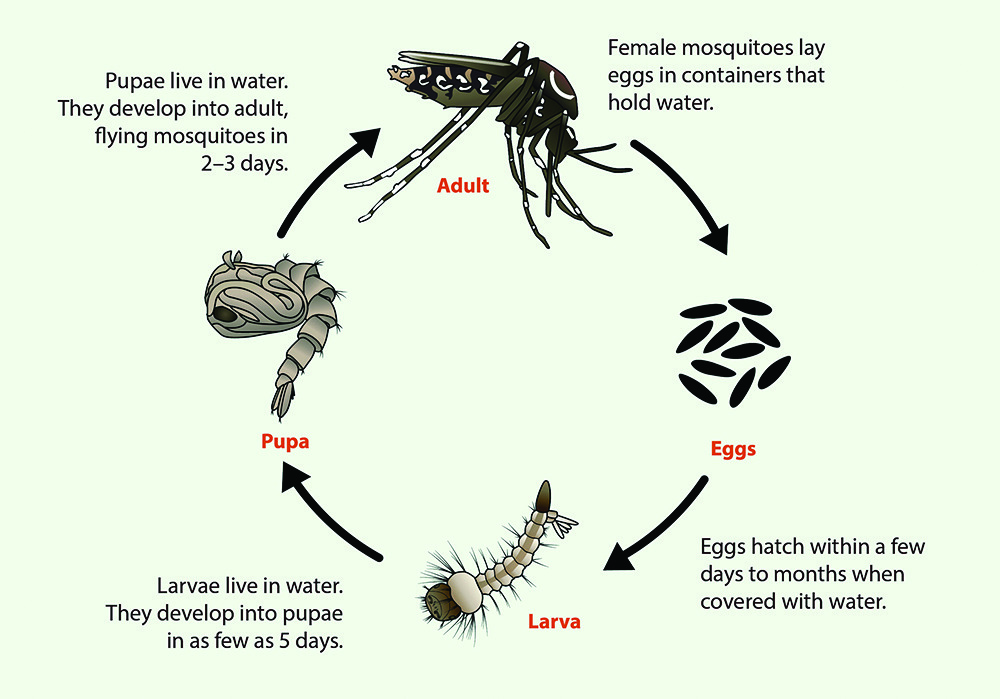
Also important is the knowledge of the breeding habits of aedes mosquito. Any pool of water is a fertile breeding ground, even egg shells and water bottle caps in garbage piles. Fumigation, as some Kathmandu wards did two months into the outbreak last year, was ineffective because the virus was already spreading from already-infected people.
In short, destroying the larvae by removing possible breeding sites is the best preventive measures. “Every step that the government took last year after the onset of the pandemic, take them now. In fact, the people should pressure their local governments to do so right away,” adds Basnyat.
Unlike Covid and most other infectious diseases, a dengue reinfection is even more dangerous and can be fatal. Writing in the journal The Lancet in 2020, authors Sudeep Adhikari, Buddha Basnyat and Kripa Maharjan explain: ‘Primary infection with any serotype in a non-immune population generally causes mild disease. When secondary infection with another serotype occurs in the same population, there is antibody-dependent enhancement, which usually causes severe dengue. Over time, this secondary infection might lead to a so-called explosion of the disease.’
Such an explosion occurred in 2022 in Nepal’s urban areas, affecting mostly children and young adults. Misdiagnosis also caused complications in patients. Hospitals were overwhelmed and many patients had to be turned away. There was rampant overtreatment, often with antibiotics which are ineffective against viruses.
With global warming, disease vectors like mosquitos and the virus are also moving to higher altitudes spreading not just dengue but malaria, kalazar and chikungunya.
Additional reporting by Ritika Tewari.

