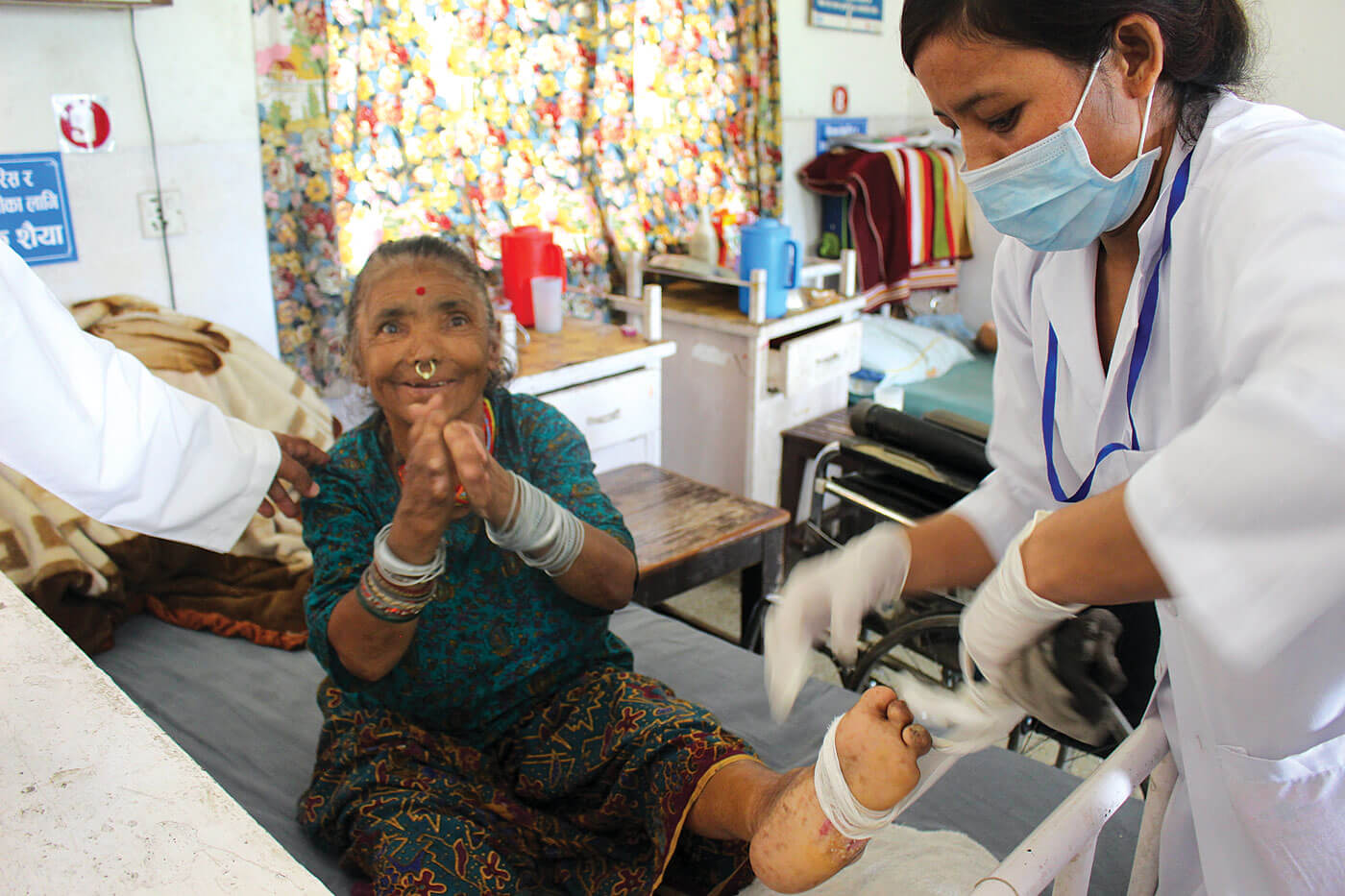
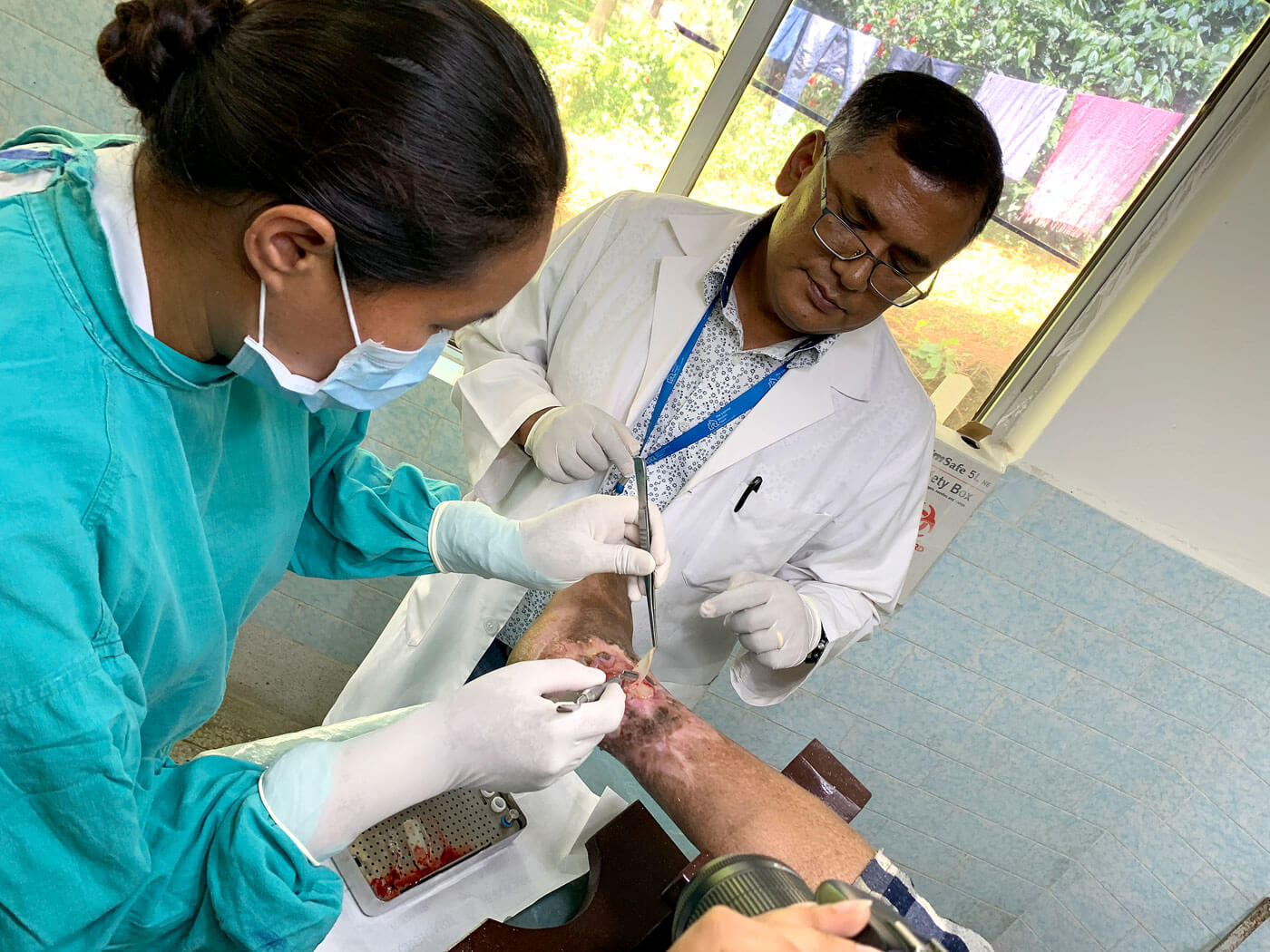
No one would argue against Nepal needing to boost its budget for public health, but given the low allocation and poor management of government hospitals, the question arises: what do we do until politicians get their priorities right?
Over the past few decades, health expenditure in Nepal has been consistently less than one-tenth of the nation’s GDP. If it was not for community level work by Female Community Health Volunteers and the effort of dozens of nonprofits medical care would be beyond the reach of most Nepalis.
At present, 70% of the medical expenditure for people is met out-of-pocket. There are many instances where even middle-class households are pushed below the poverty line because they have to use all their savings, sell property or borrow money to meet hospital expenses of family members.
When health financing relies heavily on such payments, people fall into the ‘medical poverty trap’, as their treatment costs are uninsured and expenses not reimbursed.
In remoter parts of Nepal, families have had to sell property even to pay for fractures or simple operations for relatives who have to be taken to private city hospitals.
Non-profits and international charities have stepped in to fill the gap left by the government’s incapacity to make quality healthcare more affordable and accessible. Stable healthcare infrastructure therefore relies on non-government funding and altruistic intervention.
Subsidies by not-profits can be seen in virtually every sphere of healthcare in the country. From primary healthcare centres in the countryside to high-end hospitals in the cities, many would not be able to function without support from charitable organisations. The partnership is largely financial, and usually pay for services in underserved areas of the country for excluded communities.
Bayalpata Hospital, in Accham district, for instance, is a model public-private partnership that can thrive when state-of-the-art medical interventions are melded with philanthropy. This government-owned hospital is managed by Nyaya Health Nepal (NHN) and provides absolutely free healthcare for 100,000 patients annually.
In Kathmandu valley itself, the Nepal Cleft and Burn Center at Kirtipur Hospital is providing valuable service for cleft palate surgery and treatment of burns patients, and is run by a non-profit. It is Nepal's first teaching hospital specialising in deformity-correction reconstructive surgery.
Anandaban Hospital in Lalitpur run by The Leprosy Mission, is one of South Asia’s finest facilities for leprosy treatment, and receives many referrals from in and out of Nepal every year. It uses a new technique called Leukocyte Platelet Rich Fibrin (LPRF) that helps cure lesions of leprosy patients much faster.
United Mission to Nepal has been managing several hospitals across rural Nepal for the past 60 years, most notable being in Tansen and Okhaldhunga.
These hospitals are testament to how healthcare facilities that place philanthropy front and centre in their operational modality can deliver quality treatment better than public hospitals across Nepal.
While support from foreign non-profits has become part and parcel of a well-managed hospital in Nepal, foreign grants alone cannot transform healthcare in every corner of the country. After all, they are just temporarily doing the government’s job. Nepal’s Constitution guarantees free basic health care for every citizen, but that has only remained a lofty unfilled goal in many parts of Nepal.
The only alternative is to build a self-sustained funding system to run medical facilities, and the easiest way to achieve this while a universal national insurance scheme comes to fruition, is to rely on domestic and international volunteerism and philanthropy.
Philanthropy is in fact deep-rooted in Nepal’s sociocultural structure and the country in fact stood 56th in the World Giving Index, 2022. This means that Nepalis are, on average, more likely to donate to charity than people in more than half of the world’s countries.
The only problem is that they do not have much money to spare, and whatever they give is not enough to take care of the enormous burden of need.
Channeling locally raised funds into innovative healthcare projects through philanthropic organisations is one way to go about encouraging local giving. The problem lies in that local donors, because they do not trust Nepali charities resist donating institutionally.
Corporates that would like to donate are also held back because there is no provision for tax deductible donations to charity – possibly because the government does not have a transparent way to ensure that it will not be misused.
This has propelled hospitals and health projects in Nepal to turn to external, international sources of funding. One example is the Nick Simons Institute (NSI) that backstops 44 hospitals and health care centres across Nepal because its founder had a special personal attachment to Nepal.
Outside funding also inhibits Nepali donors who think there is plentiful foreign funds. To change this dynamic, Nepal needs to alter the culture of giving.
This change starts by building local trust. If local donations are to be pooled effectively, their givers need to trust healthcare projects and believe in the value they will create. This comes along with the need for the state to strengthen tax incentives to encourage philanthropic giving.
But aside from local individuals and communities, for-profit companies also have a major role to play. In 2017, when Nepal Rastra Bank mandated banks and financial institutions to use at least 1% of their net profits for philanthropic activities, it was a major step to encourage corporate altruism.
A 2021 survey conducted by the Nepal Rastra Bank found that 41% of banks and financial institutions in a sample expressed commitment to support various deprived sectors, with health being the second most popular choice after education. However, these companies need to find more ways to engage in Corporate Social Responsibility activities focussed on healthcare.
This may include incentivising doctors to serve in remote locations where urgent medical attention is most needed, investing to upgrade teaching methodologies and improve access to medical literature, supporting non-mainstream illnesses such as autism and dementia, and subsidising follow-up health checks instead of one-time health camps aimed purely for image building.
Healthcare innovation is another area where funds are needed since the government is not fulfilling its mandate. As digitisation dominates healthcare, there is a need for modern healthcare infrastructure, including research and innovation centers to innovate.
But more pressing is that access to even basic health facilities remains a formidable challenge in rural Nepal. Local philanthropy, from individuals, communities, and companies allows local context and culture to shape health projects, increasing community ownership. It leverages the collective interests of local donors, making them feel directly involved in development.
Local funding has the added benefit of kindling trust among rural people in the healthcare infrastructure they invest in. Transparent philanthropy can encourage rural communities to seek services from these establishments. This may further discourage informal at-home diagnosis and witch-doctor consultations, which a recent study in Humla found was the case for 50% of patients in the district.
To be sure, it is not that the government has not made efforts. In public hospitals, primary healthcare is free of cost. But it only covers very basic services. Most hospitals are overcrowded, and lack minimum service standards.
Private hospitals are state-of-the-art and provide international standard medical care, but are so expensive that they are out of reach of most Nepalis.
Local altruism, could bridge the gap between these two extremes. It can fill the healthcare need, but also nudge the government and private sector to prioritise quality care over all else.
Yugottam Koirala and Yugeshwor Koirala are twins, and are from the Punyaarjan Foundation.