
Looking at the daily statistics from the Ministry of Health, the figures are alarming. Nepal is nearing the 100,000 Covid-19 cases mark, and this week the country overtook the total number of cases in China.
Kathmandu Valley has emerged as a major hotspot since August-September and now accounts for one-third all Covid-19 deaths and over 61% of active cases nationwide.
This is a dramatic about-turn from July, when the Valley accounted for only 4% of all active cases in Nepal. But by August it was up to 15%, and 34% in September.
On Wednesday, Nepal recorded its highest number of positive cases on a single day with 3,439, out of which 1,684 were in Kathmandu Valley alone. Fifteen people died in the past 24 hours, bringing the total fatalities to 578.
The number of active cases on Wednesday also crossed the 25,000 threshold, which the Ministry of Health had warned would overwhelm Nepal’s health infrastructure and a lockdown may need to be re-imposed.
Currently, 233 patients are being treated in ICU and 37 are on ventilator support. Bagmati province has 127 patients in ICU and 25 on ventilators.
Nepal’s health infrastructure is far from being overwhelmed by Covid-19 patients. There are an estimated 2,600 ICU beds in private and government hospitals nationwide, and of the 900 ventilators in hospitals 490 are in working order.
The problem is that there is uneven distribution of these facilities. There are not enough ICU beds where they are needed most, and beds available in private hospitals tend to be unaffordable to most Nepalis.
The government’s 25,000 threshold appears to be a deliberate strategy to convince people to adopt preventive measures to control the disease, since curative capacity is limited. In Wednesday’s press briefing, the Ministry of Health did not say anything about a re-imposition of the lockdown.
Bir, Teaching, Teku and Patan are the only government-run hospitals in Kathmandu Valley admitting seriously ill Covid-19 patients, and their limited capacity is getting saturated. All 20 ICU beds in Teku are occupied, so are 10 beds in Bir Hospital, 20 in Teaching and 22 in Patan that are set aside for Covid-19 patients.
The Armed Police Force (APF) hospital also designated for Covid-19 care has a 20-bed ICU, but only half are in operation because of the lack of trained healthcare workers.
Some private hospitals in Kathmandu Valley like Star, MediCiti, Grande, Norvic, HAMS and B&B also admit Covid-19 patients, but these are expensive and have only a part of their total beds designated as Covid-19 wards.
Because of the pandemic, many non-Covid-19 patients are not seeking treatment, and private hospitals are converting existing capacity to coronavirus wards to compensate for the loss of revenue.
For Samir Adhikari at the Ministry of Health, the limiting factor is not ICU beds but adequate supply of oxygen. He says: “Most patients do not need to be in ICU or have a ventilator, they need oxygen and it is much more critical to ensure that there are enough cylinders.”
Adding to the problem is that patients without major complications have also occupied ICU beds, there is a poor referral system, shortage of drugs, mismanagement of human resources and facilities.
Since June, more than 350 healthcare professionals have been trained by the National Health Training Centre in critical care, and are now working in various hospitals and institutions across the country, but not in ICU wards.
“We submitted the details of the trained professionals to the ministry and it is now their responsibility to deploy them where they are most needed,” says director of the Centre, Yaduchandra Ghimire.
The Ministry of Health sent a budget to all government hospitals to repair ventilators, install ICU beds and oxygen generators. However, it does not look like this has been done.
Director General of Health Services Dipendra Man Singh says: "We have to move fast. At the rate Covid-19 infection is spreading, it is becoming increasingly difficult for even Kathmandu to manage the treatment of infected patients.”
This situation was not unexpected. Last month, the Nepal Society of Critical Care Medicine had suggested the Health Ministry to establish 500-bed medical college with 50-bed ICU for a possible surge in symptomatic patients.
"Infected people are now dying at home without treatment. The infrastructure needed to treat critically ill patients has not been managed due to the conflicting interest of the leadership at the health ministry," says one doctor affiliated with the group.
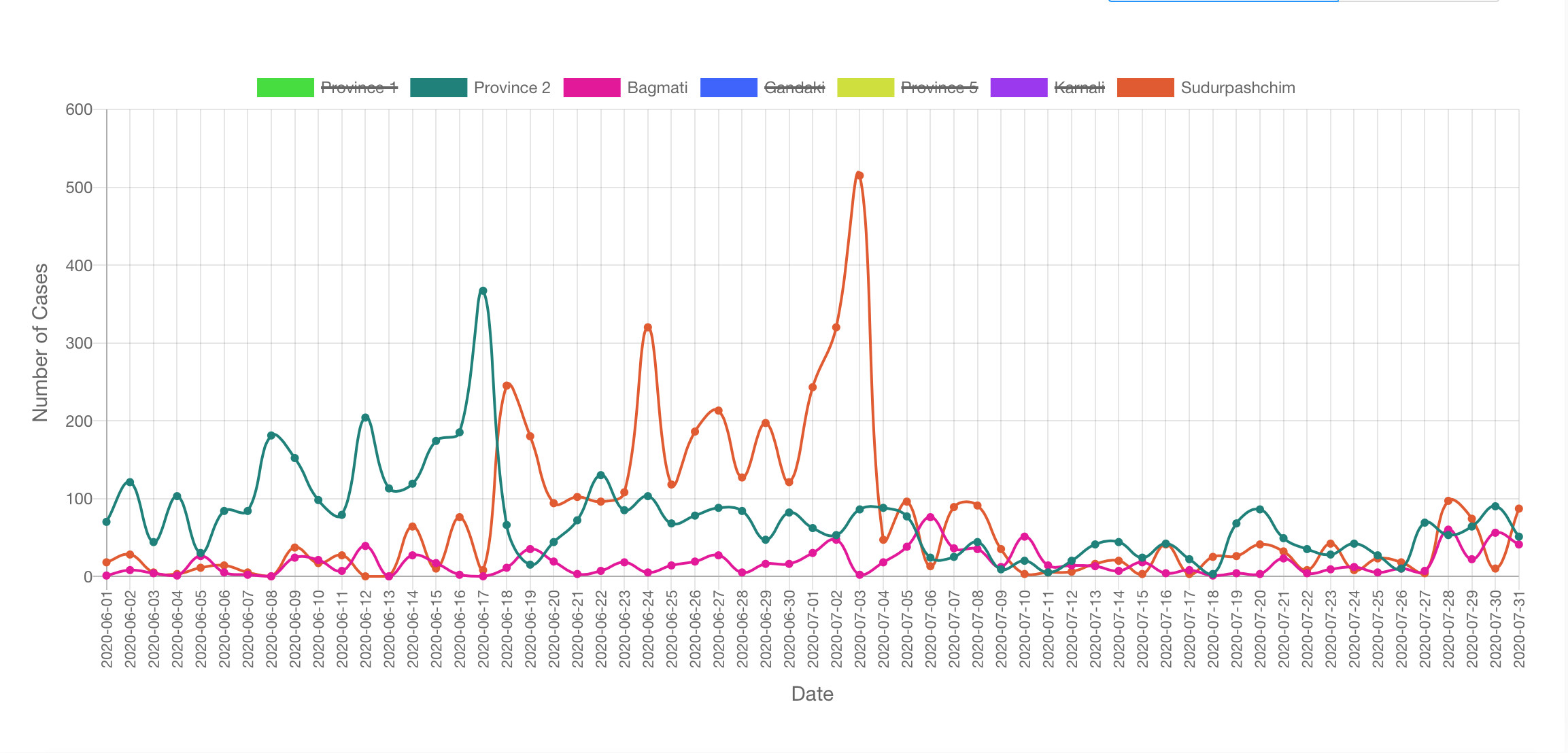
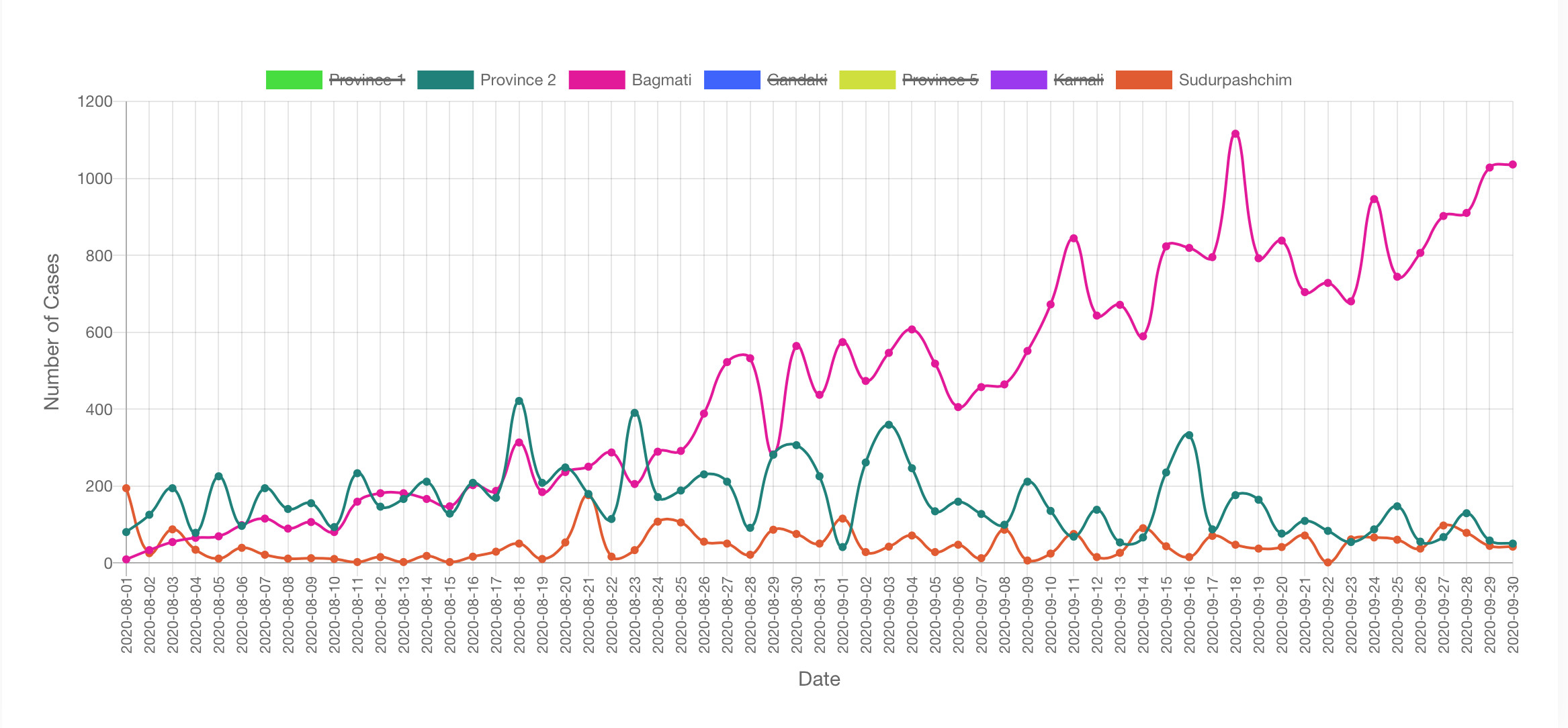
While Kathmandu Valley’s hospital capacity is stretched, things have more or settled down in Province 2 and Sudur Paschim Province that saw multiple peaks back in June-July (see graphs, above) following the return of migrant workers from India. Hospitals there were also overwhelmed then, but now able to manage patients.
Additional reporting by Ramu Sapkota.
