
Last November, a speeding bus in Argakanchi lost control and tumbled down a mountain, killing 19 and injuring 18 passengers. Three weeks later, another bus careened off a serpentine road in Sindhupalchok, killing 16 and wounding 18.
Seven Nepalis die every day in road and highway accidents. Shocking though that statistic might be, the number of injured is much higher. On average, 40 people are injured on roads across the country each day. Last year, there were nearly 13,000 road accidents in which 2,736 people lost their lives and 10,731 were seriously injured.
Read also: It’s an emergency: Nepal needs to improve trauma care, Sanghamitra Subba
Highway accidents are now the biggest killer of young men and women in the country. The causes are usually carelessness and speeding, and poorly-maintained roads and vehicles. The number of accidents are rising faster than the increase in the number of vehicles.
Those who survive often have traumatic brain and spinal cord injuries, requiring long-term or life-long rehabilitative care. But the state of rehabilitation in Nepal is nearly non-existent. There is no government rehabilitation centre, and while some private hospitals do offer inpatient physiotherapy, none have dedicated acute rehabilitation units and none employ physical medicine and rehabilitation consultants.
“Forget about prioritising it, rehabilitative medicine is not even included in the healthcare system of Nepal,” laments Raju Dhakal, the only physical medicine and rehabilitative doctor registered in Nepal. “Every hospital has a cardiology unit, intensive care unit and even physiotherapy but no rehabilitation unit. This should be integrated in the healthcare system rather than treated as a separate entity.”
The Spinal Injury Rehabilitation Centre (SIRC) in Sanga, founded in 2002, is Nepal’s largest inpatient rehabilitation centre and the only one specialised in spinal cord injury. The 51-bed hospital treats patients from all 77 districts and provides inpatient rehab for 300 individuals a year.
It also conducts outpatient care, home follow-up visits, community outreach programs, and a residential vocational rehabilitation program to help people with disabilities integrate back into society and to better equip thier families to deal with their special needs.
The only other facilities with dedicated inpatient rehabilitation beds are Green Pastures Hospital in Pokhara and the Hospital for Rehabilitation and Disabled Children in Kavre.
“Usually two physical medicine and rehabilitation specialists are needed for every 100,000 people. This means we need 500 specialists in Nepal, and instead we have one,” says Manoj Sivan, associate professor of rehabilitative medicine at Leeds University in the UK, who says the gap in rehabilitative care can be bridged with telemedicine.
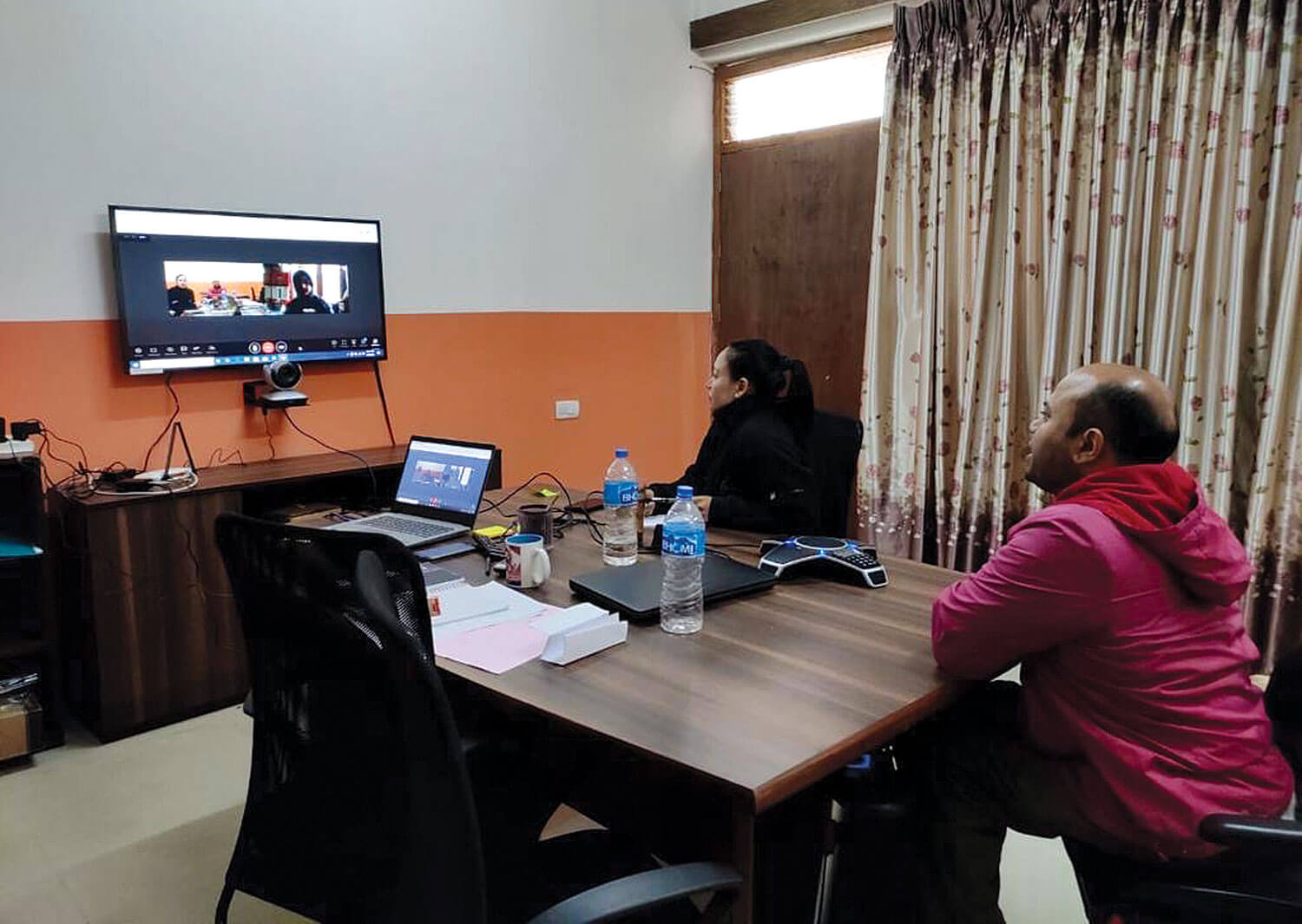
“Tele-rehabilitation can link the people in the community with specialists to provide necessary interventions remotely, allowing them to the save time and money spent travelling to the centre,” adds Sivan, who was in Nepal last month with a team of researchers to launch a six-month pilot project called Tele-rehabilitation Nepal (TERN) in collaboration with SIRC (above).
Unlike other telemedicine consultations where a patient has to visit a health post to connect with doctors based in cities, in tele-rehab a social worker from SIRC visits patients, finds out their needs and then connects them with a specialist team that consists of a physician, physiotherapist, occupational therapist, nurse and psychologist.
Patients with long-term disabilities and their families learn about better management of bladder, bowel and pain, as well as exercise techniques to help mobility.
The idea for e-rehab first came to Dhakal when a paraplegic patient from Surkhet visited SIRC and was unable to pay a minimal consultation fee. She had spent Rs45,000 to hire a jeep and had to pay for extended hotel stay for herself and two relatives. “It hit me hard,” Dhakal recalls. “This country’s topography makes accessing healthcare stressful for most Nepalis.”
Besides those with spinal injuries caused by highway accidents, tele-rehabilitation is useful for those recovering from other medical emergencies like strokes and also for general medicine.
The Nepal Government’s 2016 Policy, Strategy, and Ten Year Action Plan on Disability Management plans for every province to have at least one fully equipped rehabilitation centre and established orthotics/prosthetics workshop in the next ten years. SIRC is also working with the Ministry of Health to develop another 100-bed hospital to provide specialised rehabilitation care.
Added Dhakal: “Sooner or later the government has to take responsibility and decentralise rehabilitative care. This will allow us to train more people and supervise other centres to decentralise rehab.”
Wheelchair doctor treats patients in wheelchairs
As the only physical medicine and rehabilitation doctor in Nepal, Raju Dhakal (left) has a lot on his plate. His days are packed with back-to-back consultations with rehabilitation patients. The 37-year-old does this with ease as he moves about in his wheelchair greeting patients at Spinal Injury Rehabilitation Centre (SIRC) at Sanga, Kavre.
Dhakal himself was diagnosed with poliomyelitis when he was two-and-half years old. Originally from Gorkha, he came to Kathmandu and lived in SOS Children’s Village while undergoing treatment. He started school at age seven, and learned to read and write at the same time as he learned to use crutches.
Read also: New life for Khagendra B Basnyat, Sewa Bhattarai
With an MBBS from Kathmandu Medical College, Dhakal went on to receive an MD in Physical Medicine and Rehabilitation in Dhaka.
“At daily rotations during my internship, there was one patient that every doctor skipped. He was undergoing rehabilitation after treatment for a spinal injury. No one could do anything for him so he remained there in a corner of that ward,” recalls Dhakal. “This opened my eyes to a gaping hole in medical care in Nepal.”
Dhakal went on to become honorary clinical fellow at the Department of Rehabilitative Medicine at the Royal Melbourne Hospital in Australia. He trained in Spinal Cord Medicine and Rehabilitation in Ireland, Canada and Switzerland.
“In Nepal we are still very focussed on diagnosis and acute treatment. But what about residual paralysis in case of trauma, traumatic brain injuries and spinal injuries?” asks Dhakal. “Long-term rehabilitative care for patients with disabilities is severely lacking. We need more facilities for specialised rehabilitation care.”
