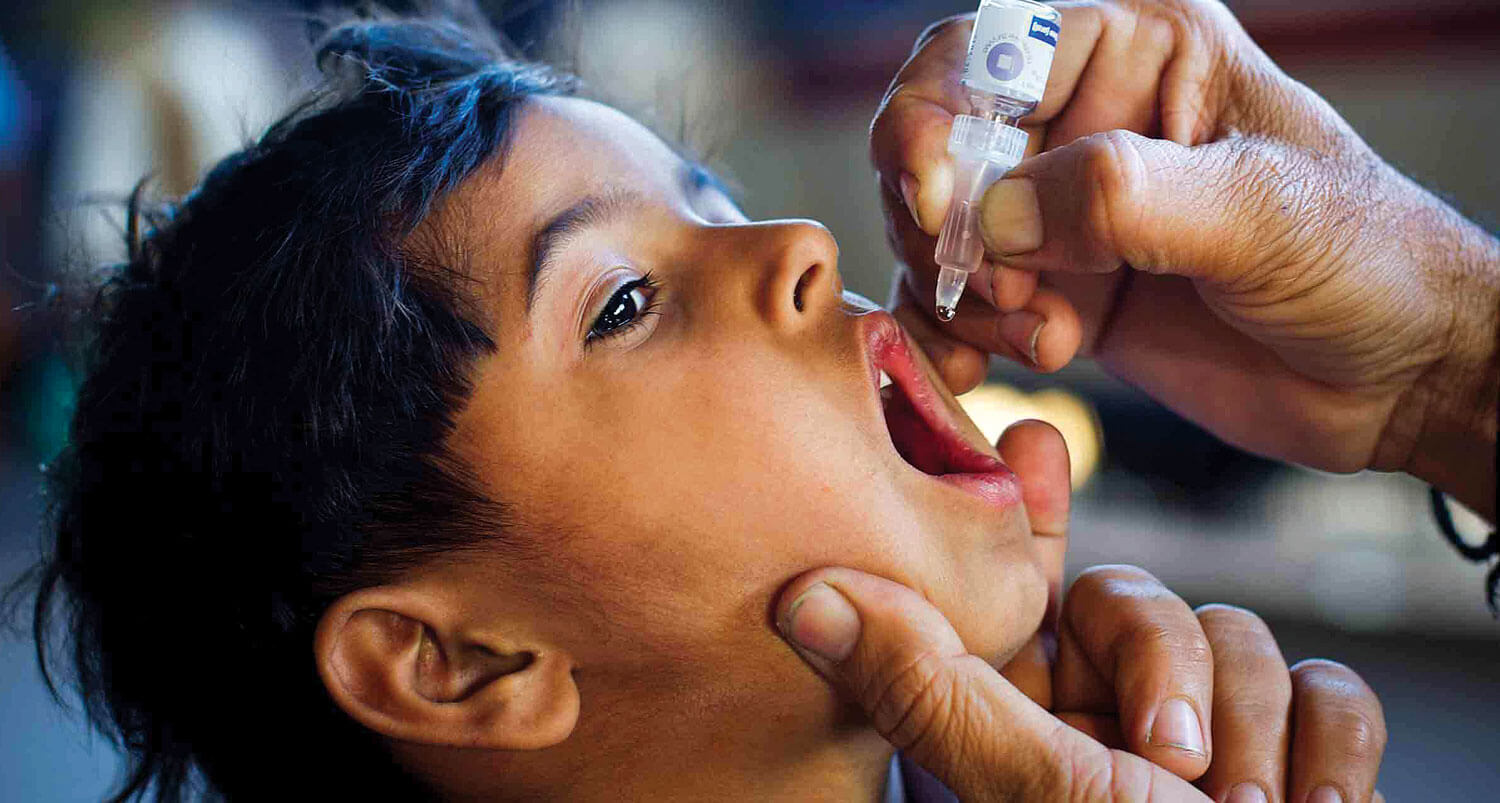
Last month, the prestigious New England Journal of Medicine published a study of the successful trial of a new typhoid vaccine that could prevent thedeaths of many children around the world. The vaccine research was conducted at Patan Hospital by a Nepali researcher.
The randomised control trial of the typhoid conjugate vaccine (TCV) was conducted among more than 20,000 participants in Lalitpur district, and the efficacy of the new vaccine was found to be 81.6% -- a major improvement on previous vaccines. (See box below).
The positive news from Nepal came as various parts of the world, including the US, Europe, Samoa and Africa, struggled to cope with the biggest measles outbreak in decades. Most of the cases have now been associated with people forgoing recommended preventive shots because of fears of side-effects fanned by social media.
Fear of vaccination started ever since a paper in 1998 in the medical journal The Lancet cited a link between autism and the measles, mumps, rubella (MMR) vaccine. The research was later found to be fraudulent and retracted, but the anti-vaccine movement gained traction again in the past year after the rumours resurfaced on the Internet resulting in families rejecting early childhood immunisation against diseases like polio, rubella and measles.
“The good news is that unlike in the rest of the world, people in Nepal demand vaccines. If we miss to vaccinate a child for any reason, parents come knocking, asking for the shots,” says Jhalak Gautam of the Family Welfare Division at Teku.
Sameer Mani Dixit of The Centre for Molecular Dynamics Nepal concurs. “Entire communities actively participate in vaccination programs and are well aware of the benefits. Every mother in Nepal knows the immunisation schedule by heart.”
The Centre for Molecular Dynamics Nepal has just completed a study on why the country has been so successful with its immunisation program, and the results will be published later this month. This study and similar studies underway in Senegal and Zambia are being conducted with funding from the Bill and Melinda Gates Foundation, in an effort to analyse the success of vaccination programs in developing nations.
Nepal’s national immunisation program started in 1988 and now vaccinates some 620,000 children under 15 months of age every year against 11 infectious diseases such as tuberculosis, polio, pneumonia and measles.
The last case of polio was detected in Rautahat district in 2010, and Nepal was declared polio free four years later. The country also eliminated maternal and neonatal tetanus in 2005. Similarly, Japanese encephalitis, diphtheria, pertussis and pneumonia have all been controlled, and there are regular vaccinations against congenital rubella syndrome and hepatitis B.
Despite the high immunisation rate, thousands of Nepali children continue to die due to easily preventable and treatable communicable diseases like diarrhoea and according to Nepal Demographic Health Survey 2016, one in a hundred Nepali children have still not been vaccinated against any infectious diseases.
Read also: "Nepal is a microcosm of all the change in world health"
Immunisation coverage data from last year also shows a worryingly high dropout rate. While 93% of newborns received BCG jabs, the first in the national immunisation schedule, the coverage dropped to 73% by the time children received the last vaccine, an immunisation against measles and rubella, recommended at the age of 15 months.
Several cases of measles have been detected in Kapilvastu, Dang, Makwanpur, Sarlahi and Manang districts recently, and Nepal has not been able to meet its previously set target to eliminate measles and rubella by 2019. The new goal is to eliminate the diseases by 2023.
“Dropout rate is a challenge, we have not been able to reach the remotest corners of the country, and children miss their shots because of migration,” says Jhalak Gautam. “We now have a strategy to identify missed pockets and deliver shots at home if required.”
The Immunisation Section of the Ministry of Health is now gearing up for a nation-wide measles-rubella vaccination campaign aimed at those who might have missed routine shots. Three million children between the ages 9 months to 5 years are expected to participate in two phases of the campaign later this year.
Polio drops will also be administered at the same time to 1.5 million children under five in 19 Tarai districts. The Immunisation Section is also introducing a new vaccine against rotavirus this June to reduce the prevalence of childhood diarrhoea.
The new challenge to vaccination comes from an unlikely quarter: federalism. There is confusion about where the vaccines are sourced and who should pay for them. There is concern about the quality of vaccines, many of which need a cold chain with refrigeration to the point of delivery.
Warns Patan Hospital physician Buddha Basnyat: “Nepal’s immunisation program is a model of success, but we cannot afford to be complacent.We have to introduce newer and more effective vaccines while also prioritising hygiene and sanitation simultaneously.”
Successful trial of new typhoid vaccine
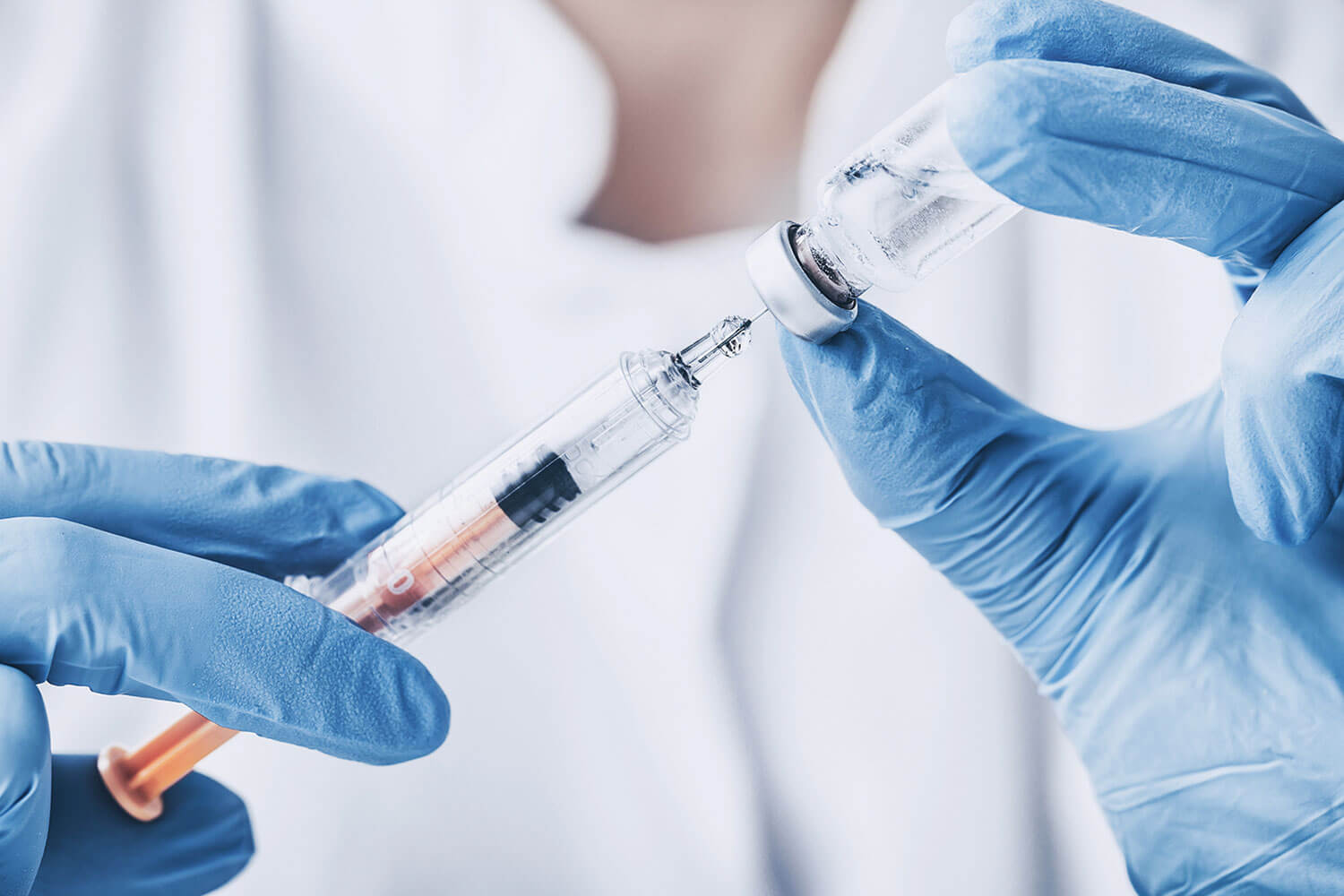
Over 20,000 children between 9 months and 16 years of age in Lalitpur district participated in the first large-scale randomised controlled trial of a new vaccine against typhoid, a disease that affects millions across South Asia.
Half of them received the vaccine and the other half received control shots. The efficacy of Typhoid Conjugate Vaccine (TCV) was found to be 81.6%, and the results were published last month in the prestigious New England Journal of Medicine.
Prior to this, a small-scale TCV trial was conducted in Britain, and the World Health Organisation (WHO) has since strongly recommend the use of the vaccine for countries and regions where the water and food-borne infection is most common. "Pakistan has been able to control typhoid with this vaccine and Vietnam has eliminated it," says lead author of the paper, Mila Shakya, "Administration of this new, effective vaccine by our government will help control the most common bacterial disease in Nepal and South Asia."
Typhoid is a contagious infection caused by the bacteria Salmonella typhi, which is found in contaminated food and water and which causes fever, diarrhoea and vomiting. It can easily be prevented with awareness, safe drinking water and frequent hand-washing.
The vaccine is useful because it is a prophylactic in places where preventive measures are taking time to implement. There are some 21 million typhoid cases and 161,000 typhoid-related deaths annually worldwide. South Asia has been often dubbed as the hub of typhoid and there are some 500 cases per 100,000 population in the region.
“This study is Nepal taking a lead in preventing typhoid, after never having really prioritised it. It might not kill as many people as other diseases do, but it still affects thousands of school-going children,” says physician Buddha Basnyat at Patan Hospital.
TCV is not the first typhoid vaccine to be developed. Currently there is an injectable unconjugated polysaccharide vaccine for persons aged two years and above, and an oral capsule for those over six years of age. But they do not work well on young children and they provide protection only for a few years. TCV on the other hand can be given to children below 2 years and the immunisation lasts up to five years.
“A single dose of the new vaccine is safe, immunogenic, and effective, and the deployment of the vaccine will reduce the burden of typhoid in high-risk populations,” stated the interim analysis. “This new evidence of efficacy is especially timely with the recent spread of extensively drug resistant typhoid fever, which threatens child health in affected regions.”
Pakistan, which has been struggling against an outbreak of drug resistant typhoid fever since 2016 is already using TCV with positive results and its Sindh province will become the first region in the world to include TCV in routine childhood immunisations.
Gavi, the Vaccine Alliance, which has earmarked $85 million to fund the introduction of the vaccine in the world’s poorest countries, is supporting the program. Nepal is also eligible for funding from the alliance.
Says Basnyat: “We should take action before we are also hit, like Pakistan, by the drug-resistant typhoid. What are we waiting for, when Gavi is ready to fund the vaccination program for free and its benefits are so clear. This is a case of vaccine under-utilisation.”
Sonia Awale
